Cardiovascular Biomaterials Engineering and Translational Research
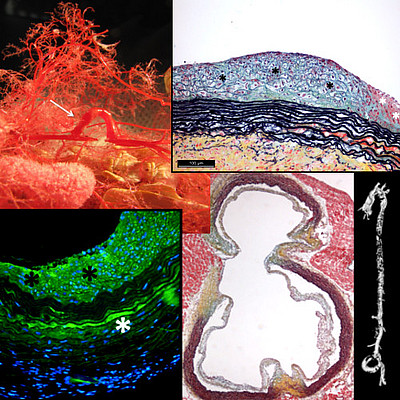
Cardiovascular pathologies, such as heart valve disease, atherosclerosis or myocardial insufficiency, are the leading reasons for mortality in industrialized parts of the world. Advanced disease stages require tissue repair or replacement by implants such as heart valve prostheses.
The Cardiovascular Biomaterials Engineering and Translational Research Group of the Department of Cardiovascular Surgery, headed by Prof. Dr. med. Alexander Assmann, has set its focus on the development, characterization and translational evaluation of naturally derived scaffolds for cardiovascular applications. In particular, our interdisciplinary research projects cover the following topics:
- Development of biomaterials for cardiovascular applications
- Bio-Functionalization of cardiovascular grafts / Strategies for guided cellular population in vivo
- Evaluation of the biocompatibility and in vivo degeneration of acellular heart valve and vessel implants in functional preclinical animal models
- Investigation of the underlying mechanisms leading to the in vivo degeneration of heart valve and vessel prostheses
Current Project
Team
- Prof. Dr. med. Alexander Assmann
- Dr. med. Anna Kathrin Assmann
- Dr. rer. nat. Filip Hasecke
- cand. med. Vanessa Winnicki
- cand. med. Mikel Görzen
Previous members: Hiroshi Munakata, MD, PhD; Dr. med. Christofer Delfs; Dr. med. Kim Horstkötter; Dr. med. Kai Zwirnmann; Dr. med. Marc Struß; cand. med. Franziska Schiffer; cand. med. Friederike Heidelberg; Sentaro Nakanishi, MD; Vera Schmidt, M. sc.; Dr. med. Yukiharu Sugimura, Dr. med. Agunda Chekhoeva, Dr. med. Mahfuza Toshmatova, Dr. med. Daniel Goschmer, Dr. med. Caroline Lepke
Awards
- 2024 Ernst-Derra Research Award (by the German Society for Thoracic and Cardiovascular Surgery)
- 2023 Vascular Surgical Research Award (by the German Society for Thoracic and Cardiovascular Surgery)
- 2016 Vascular Surgical Research Award (by the German Society for Thoracic and Cardiovascular Surgery)
- 2015 Edens Award for Heart and Circulatory Research (by the Eberhard Igler Foundation)
- 2014 Ulrich Karsten Scientific Award (by the German Society for Thoracic and Cardiovascular Surgery)
Publications
- Assmann, A., Assmann, A.K., Lichtenberg, A. et al. Degeneration biologischer Herzklappen in einem SOD3-Defizienz-Ratten-Modell. Z Herz- Thorax- Gefäßchir (2024). doi: org/10.1007/s00398-024-00654-1
- Assmann, A.K., Lichtenberg, A., Assmann, A. et al. Einfluss von PPAR-γ-Agonisten auf die kalzifizierende Degeneration kardiovaskulärer Prothesen. Z Herz- Thorax- Gefäßchir (2023). doi: org/10.1007/s00398-023-00586-2
- Assmann A, Schmidt V, Lepke C, Sugimura Y, Assmann AK, Barth M, Lichtenberg A, Akhyari P. Degeneration of biological heart valve grafts in a rat model of superoxide dismutase-3 deficiency. FASEB J. 2022 Nov;36(11):e22591. doi: 10.1096/fj.202200727RR. PMID: 36251410
- Assmann AK, Winnicki V, Sugimura Y, Chekhoeva A, Barth M, Assmann A, Lichtenberg A, Akhyari P. Impact of PPAR-gamma activation on the durability of biological heart valve prostheses in hypercholesterolaemic rats. Eur J Cardiothorac Surg. 2022 Dec 2;63(1):ezad005. doi: 10.1093/ejcts/ezad005. PMID: 36629469.
- Assmann AK, Goschmer D, Sugimura Y, Chekhoeva A, Barth M, Assmann A, Lichtenberg A, Akhyari P. A role for peroxisome proliferator-activated receptor gamma (PPAR-gamma) agonists in counteracting the degeneration of cardiovascular grafts. J Cardiovasc Pharmacol. 2021 Oct 4. doi: 10.1097/FJC.0000000000001150.
- Chekhoeva A, Nakanishi S, Sugimura Y, Toshmatova M, Assmann AK, Lichtenberg A, Akhyari P, Assmann A. Dichloroacetate inhibits the degeneration of decellularized cardiovascular implants. Eur J Cardiothorac Surg. 2021 Jul 23:ezab333. doi: 10.1093/ejcts/ezab333.
- Sugimura Y, Chekhoeva A, Oyama K, Nakanishi S, Toshmatova M, Miyahara S, Barth M, Assmann AK, Lichtenberg A, Assmann A*corr, Akhyari P. Controlled autologous recellularization and inhibited degeneration of decellularized vascular implants by side-specific coating with stromal cell-derived factor 1α and fibronectin. Biomed Mater. 2019 Nov 6. doi: 10.1088/1748-605X/ab54e3.
- Toshmatova M, Nakanishi S, Sugimura Y, Schmidt V, Lichtenberg A, Assmann A*corr, Akhyari P. Influence of laminin coating on the autologous in vivo recellularization of decellularized vascular prostheses. Materials (Basel). 2019; 12(20). pii: E3351. doi: 10.3390/ma12203351.
- Iijima M, Aubin H, Steinbrink M, Schiffer F, Assmann A, Weisel RD, Matsui Y, Li RK, Lichtenberg A, Akhyari P. Bioactive coating of decellularized vascular grafts with a temperature-sensitive VEGF-conjugated hydrogel accelerates autologous endothelialization in vivo. J Tissue Eng Regen Med. 2018; 12(1):e513-e522. doi: 10.1002/term.2321. Epub 2017 May 23.
- Annabi N, Zhang YN, Assmann A, Vegh A, Cheng G, Dehghani B, Lassaletta A, Gangadharan S, Weiss AS, Khademhosseini A. Engineering a highly elastic human protein-based sealant for surgical applications. Sci Transl Med. 2017; 9(410). pii: eaai7466. doi: 10.1126/scitranslmed.aai7466.
- Sugimura Y, Schmidt AK, Lichtenberg A, Assmann A*corr, Akhyari P. A Rat Model for the In Vivo Assessment of Biological and Tissue-Engineered Valvular and Vascular Grafts. Tissue Eng Part C Methods. 2017; 23(12):982-994. doi: 10.1089/ten.TEC.2017.0215.
- Assmann A, Struß M, Schiffer F, Heidelberg F, Munakata H, Timchenko EV, Timchenko PE, Kaufmann T, Huynh K, Sugimura Y, Leidl Q, Pinto A, Stoldt VR, Lichtenberg A, Akhyari P. Improvement of the in vivo cellular repopulation of decellularized cardiovascular tissues by a detergent-free, non-proteolytic, actin-disassembling regimen. J Tissue Eng Regen Med. 2017; 11(12):3530-3543. doi: 10.1002/term.2271.
- Timchenko EV, Timchenko PE, Lichtenberg A, Assmann A, Aubin H, Akhyari P, Volova LT, Pershutkina SV. Assessment of decellularization of heart bioimplants using a Raman spectroscopy method. J Biomed Opt. 2017; 22(9):91511. doi: 10.1117/1.JBO.22.9.091511.
- Assmann A, Vegh A, Ghasemi-Rad M, Bagherifard S, Cheng G, Sani ES, Ruiz-Esparza GU, Noshadi I, Lassaletta AD, Gangadharan S, Tamayol A, Khademhosseini A, Annabi N. A highly adhesive and naturally derived sealant. Biomaterials. 2017; 140:115-127. doi: 10.1016/j.biomaterials.2017.06.004. Epub 2017 Jun 6.
- Nagy E, Lei Y, Martínez-Martínez E, Body SC, Schlotter F, Creager M, Assmann A, Khabbaz K, Libby P, Hansson GK, Aikawa E. Interferon-γ Released by Activated CD8+ T Lymphocytes Impairs the Calcium Resorption Potential of Osteoclasts in Calcified Human Aortic Valves. Am J Pathol. 2017; 187(6): 1413-1425. doi: 10.1016/j.ajpath.2017.02.012. Epub 2017 Apr 19.
- Annabi N, Shin SR, Tamayol A, Miscuglio M, Afshar M, Assmann A, Mostafalu P, Sun JY, Mithieux S, Cheung L, Tang XS, Weiss AS, Khademhosseini A. Highly elastic and conductive human-based protein hybrid hydrogels. Adv Mater. 2016; 28(1):40-49. doi: 10.1002/adma.201503255.
- Aubin H, Mas-Moruno C, Iijima M, Schütterle N, Steinbrink M, Assmann A, Gil J, Lichtenberg A, Pegueroles M, Akhyari P. Customized interface biofunctionalization of decellularized extracellular matrix: towards enhanced endothelialization. Tissue Eng Part C Methods. 2016; 22(5):496-508. doi: 10.1089/ten.TEC.2015.0556.
- Zhang YN, Avery RK, Vallmajo-Martin Q, Assmann A, Vegh A, Memic A, Olsen BD, Annabi N, Khademhosseini A. A Highly Elastic and Rapidly Crosslinkable Elastin-Like Polypeptide-Based Hydrogel for Biomedical Applications. Adv Funct Mater. 2015; 25(30):4814-4826. doi: 10.1002/adfm.201501489.
- Gaharwar AK, Avery RK, Assmann A, Paul A, McKinley GH, Khademhosseini A, Olsen BD. Shear-Thinning Nanocomposite Hydrogels for the Treatment of Hemorrhage. ACS Nano. 2014; 8(10):9833-9842. doi: 10.1021/nn503719n. Epub 2014 Oct 8.
- Masoumi N, Annabi N, Assmann A, Larson BL, Hjortnaes J, Alemdar N, Kharaziha M, Manning KB, Mayer JE, Khademhosseini A. Tri-layered elastomeric scaffolds for engineering heart valve leaflets. Biomaterials. 2014; 35(27):7774-7785.
- Assmann A, Akhyari P, Lichtenberg A. Dezellularisierte Aorten-Conduits und ihre Biokompatibilität - Optimierung in einem standardisierten Rattenmodell. Zeitschrift für Herz-,Thorax- und Gefäßchirurgie. 2014; 28:456-463. doi: 10.1007/s00398-014-1108-5.
- Assmann A, Horstkötter K, Munakata H, Schiffer F, Delfs C, Zwirnmann K, Barth M, Akhyari P, Lichtenberg A. Simvastatin does not diminish the in vivo degeneration of decellularized aortic conduits. J Cardiovasc Pharmacol. 2014; 64(4):332-342.
- Assmann A, Zwirnmann K, Heidelberg F, Schiffer F, Horstkötter K, Munakata H, Gremse F, Barth M, Lichtenberg A, Akhyari P. The degeneration of biological cardiovascular prostheses under pro-calcific metabolic conditions in a small animal model. Biomaterials. 2014; 35(26):7416-7428.
- Munakata H, Assmann A, Poudel-Bochmann B, Horstkötter K, Kamiya H, Okita Y, Lichtenberg A, Akhyari P. Aortic conduit valve-model with controlled moderate aortic regurgitation in rats: A technical modification to improve short- and long-term outcome and to increase the functional results. Circ J. 2013; 77(9):2295-2302.
- Assmann A, Delfs C, Munakata H, Schiffer F, Horstkötter K, Huynh K, Barth M, Stoldt VR, Kamiya H, Boeken U, Lichtenberg A, Akhyari P. Acceleration of autologous in vivo recellularization of decellularized aortic conduits by fibronectin surface coating. Biomaterials. 2013; 34(25):6015-6026.
- Assmann A, Akhyari P, Delfs C, Flögel U, Jacoby C, Kamiya H, Lichtenberg A. Development of a growing rat model for the in vivo assessment of engineered aortic conduits. J Surg Res. 2012; 176(2):367-375.



