Left Ventricular Assist Devices in Advanced Heart Failure “Coagulation meets Endothelium“

Background:
Continuous-flow left ventricular assist devices (LVADs) have arised as a vital therapeutic option in end stage heart failure not merely as bridge-to transplant but also as destination therapy. So why not use it as therapy in general? LVADs are associated with impaired endothelial function as well as with a dysbalance of coagulation leading to both, excessive bleeding and thromboembolic events as major stroke, respectively.
But how is this possible during LVAD support? The pathopysiologic mechanisms underlying these thrombotic events in LVAD patients are not fully understood. The implantation of a continous-flow LVAD may induce endothelial dysfunction and injury via the loss of pulsatile flow in the vasculature. It is not known, what happens with the endothelium and the coagulation system if you change the flow from pulsatile to continuous-flow pattern.
Our Aims:
The aims of this project are to what happens with the vascular endothelium and the coagulation system if you lose pulsatile flow pattern during LVAD support. We want to know whether these effects on vascular hemostasis promote thrombotic events in these patients.
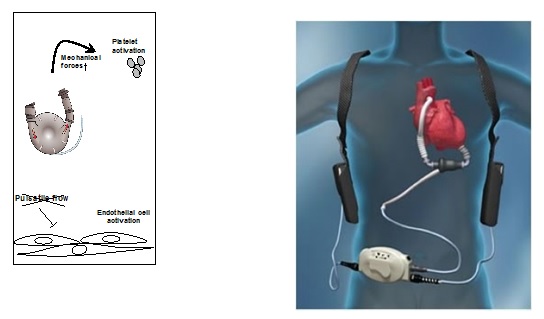
Figure 1: Sketch of platelet actication via mechanical forces generated by the assist device (LVAD) and interplay with the endothelium.
Figure 2: Current technology for wearable left ventricular assist devices (LVAD), where only the driveline, controller and batteries are outside, while impella and outflow-graft are within the thorax and even the pericardium.


